Sporadic Cavernous Angioma With Seizure
Stacie awakened in the middle of the night, just like many other nights. Only this time, as she tried to walk across the room, she became unsteady and fell into the wall. The dizziness happened again the next morning. A 36-year-old mother of four, Stacie sought medical help, but after numerous tests, the doctors were unable to provide her with a diagnosis.
One evening a year later, Stacie experienced what she later would learn was a series of partial complex seizures that included involuntary movement, a loss of awareness, and difficulty speaking. Her husband rushed her to the local hospital where a CT scan revealed an unidentified mass deep in her right temporal lobe. Stacie transferred to a larger hospital with more advanced diagnostic capabilities where she received an MRI.
Her brain mass was diagnosed as a cavernous angioma , and she was discharged on anti-seizure medication. Despite this, the seizures continued, and she sought a surgical consultation. The doctors informed her that removing her lesion would be difficult because of its deep location, and surgery could cause additional harm. Stacie needed to accept her new normal.
Says Stacie, My brain hemorrhage changed my life, but I know theres a reason. I will use it as a strength and not a weakness.
Can Developmental Venous Anomaly Cause Tinnitus
Researchers have found a new Tinnitus Cause. Watch This Video to Learn What it is. Learn the 100% Natural Tinnitus and Ear Ringing Solution and Relief. Stop Ear Ringing Now Venous malformations of the posterior fossa may cause tinnitus by their mass effect. 4 Particular attention is required in pulsatile and positional tinnitus because venous causes are frequently found. Pulsatile tinnitus that decreases with application of pressure to the jugular vein or worsens with performance of the Valsalva maneuver suggests. Tinnitus and cerebellar developmental venous anomaly. Tinnitus and cerebellar developmental venous anomaly Arch Otolaryngol Head Neck Surg. 2006 May 132:550-3. doi: 10.1001/archotol.132.5.550. Authors David Malinvaud 1 , Jean-Baptiste Lecanu, Philippe Halimi, Paul Avan, Pierre Bonfils. Affiliation 1 Ear, Nose. Tinnitus and Cerebellar Developmental Venous Anomaly velopmental venous anomaly. There was cofacial bundle and cause tinnitus
Pulsatile Tinnitus Caused By Sigmoid Sinus Dehiscence Or
Pulse-synchronous tinnitus is caused by perception of a vascular somatosound that may originate from vascular structures within the cranial cavity, head and neck region, or thoracic cavity and is transmitted to the cochlea by bony or vascular structures. 1 -3 Pulse-synchronous tinnitus can be classified as arterial, arteriovenous, or venous. On further questioning she revealed transient visual obscurations and pulsatile tinnitus. The CT scan of the brain was normal, the lumbar puncture showed increased pressure but normal cerebrospinal fluid, and the MR scan and MR venogram was reported showing a small area of developmental venous anomaly in the left parietal region but no venous. Synopsis: Pulsatile tinnitus is usually due to an ipsilateral venous anomaly that can be diagnosed with CT angiography and venography in most cases. Sources: Krishnan A, et al. CT arteriography and venography in pulsatile tinnitus: Preliminary results tinnitus, and Dauman and Tyler’s criteria are suf ficient for this purpose. Origin of Tinnitus: Somatic Versus Neurophysiologic By definition, the perception of tinnitus results from activity in the auditory nervous system. The neural activity that is perceived as tinnitus can be referred to as a tinnitus neural signal. As for most sound
Also Check: Connect Phonak Hearing Aids To Iphone
Developmental Venous Anomaly Or Dva Neuroangio
Vascular causes of tinnitus include both venous and arterial anomalies. A review of 100 cases of pulsatile tinnitus by Sismanis and Smoker 3 revealed that atherosclerotic carotid artery disease accounted for 15% of such cases. The only more common causes were benign intracranial hypertension syndrome and glomus tumors of the middle ear Dual compression of the REZ by veins and arteries is also associated with HFS, but venous origin alone is rarely reported. There are only few cases described the HFS associated with the brainstem developmental venous anomaly , also known as cerebral venous angioma. We present a rare case of HFS caused by the brainstem.
Image Findings In Brain Developmental Venous Anomalies
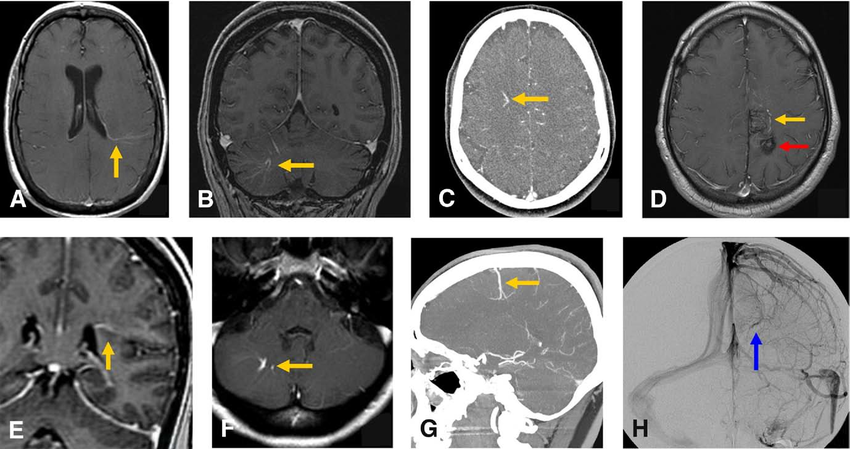
Department of Neurosurgery, Seoul Paik Hospital, Inje University College of Medicine, Seoul, Korea.
Corresponding Author: Myoung Soo Kim, MD. Address: Department of Neurosurgery, Seoul Paik Hospital, Inje University College of Medicine, 85 Jeo-dong 2-ga, Jung-gu, Seoul, Korea, 100-032. Tel: 82-2-2270-0032, Fax: 82-2-2270-0573,
Recommended Reading: How Do You Say God In Sign Language
Symptoms Of Venous Angioma
Any new formation that forms in the internal space of the human body takes a certain amount, which it “steals” from nearby organs. Therefore, the symptoms of venous angioma are as follows:
- The different frequency, intensity and nature of the pain in the head area.
- Increased dizziness, which provokes the appearance of nausea and cause vomiting reflex.
- Appearance of epileptic seizures.
- The appearance of a noise veil in my head.
- Development of problems with the circulatory and cardiovascular system.
Should I Have Concerns About Pregnancy With A Cavernous Angioma
At this time, experts believe women are no more at risk for hemorrhage during pregnancy than at any other time. But, a bleed during pregnancy can present challenges. Brain surgery to remove a cavernous angioma during pregnancy is very rare but is undertaken in cases where a second hemorrhage would be life-threatening. Women with cavernous angioma can have a vaginal delivery if they have not had a recent hemorrhage. If your doctor suggests an MRI during your pregnancy, your MRI should not include gadolinium contrast. Women who have epilepsy and are on anti-epilepsy medications should talk with their doctors about the choice of medication and folate supplementation. Ideally, you should have this conversation before you become pregnant to prevent harm because some antiepilepsy medication can increase the risk of birth defects when taken in the first weeks of pregnancy. However, having a seizure during pregnancy can cause harm that is far more serious to the fetus. Its important to continue antiepilepsy medication during pregnancy if you have had seizures and are pregnant.
Don’t Miss: How To Do The Abc’s In Sign Language
Venous Angioma In Basal Nuclei
This type of pathological lesion – venous angioma in the basal nuclei – is manifested by symptoms that have already been described more than once. Therefore, only an experienced specialist should differentiate the problem and localize it. When such a pathological symptomatology appears, urgent medical consultation is necessary.
What Is An Incidental Cavernous Angioma
Your doctor may have discovered your cavernous angioma when you had brain or spinal imaging for a reason not related to your cavernous angioma. For example, you may have received a CT scan or an MRI after a car accident or concussion. In this case, doctors will call your cavernous angioma an incidental finding. Research has shown that incidental cavernous angiomas that have not had a previous hemorrhage have a very small chance of ever becoming problematic. While you may want to follow the precautions listed in the Hemorrhage section of this booklet, you may not need repeat imaging unless instructed by your doctor or you develop symptoms. However, many doctors and patients choose to have imaging, typically with MRI, to monitor the lesion. For example, your doctor may order imaging during pregnancy, after medication changes, if another illness is diagnosed, or at times of dramatic lifestyle change, which can include extreme or unusual exercise.
Read Also: Widex Bluetooth
Tinnitus And Cerebellar Developmental Venous Anomal
In addition, venous abnormalities can also cause vascular-related PT, and these include jugular bulb abnormalities8 or the presence of vestigial veins9 as well as developmental venous anomalies.10 In addition, in recent years there has been an increasing recognition of other venous sinus lesions and PT, including a strong association with. Developmental venous anomalies, also known as venous angiomas or venous malformations, are a form of vascular malformations of the brain. Although the formation is abnormal, the veins are still able to drain blood from the brain properly. Common symptoms reported by people with developmental venous anomaly
Background and Purposeâ Although it is generally accepted that developmental venous anomalies are benign vascular malformations, over the past years, we have seen patients with symptomatic DVAs. Therefore, we performed a retrospective study and a literature study to review how, when, and why DVAs can become clinically significant This can be seen in patients with otosclerosis, middle ear effusion, and superior canal dehiscence. Additionally, abnormalities of the venous sinuses can lead to pulsatile tinnitus usually tinnitus. Tinnitus may be present for months or years before hearing loss or vertigo is noticed. The tinnitus is unilateral in 95 per-cent of cases.It is continuous and less disturb
What Is A Cavernous Angioma
Cavernous angiomas are also known as cavernous malformations and cavernoma. They are made of abnormal blood vessels. They are not cancerous. Cavernous angiomas are made of the smallest blood vessels, called capillaries. They resemble mulberries and have very thin walls compared with other blood vessels. Blood moves through them very slowly. The thin vessel walls can be leaky and can allow blood into the surrounding brain or spinal cord tissue. We believe about one in every 500 people have a cavernous angioma, but most people never have symptoms. Of the people who have a cavernous angioma, we believe many will never have a symptomatic hemorrhage.
The rarest place for a symptomatic cavernous angioma is in the spinal cord. A spinal cord cavernous angioma is not the same as a spinal hemangioma, which is located in the vertebra . Cavernous angiomas may also occur in the area of the brain called the brainstem. Spinal cord and brainstem cavernous angiomas can cause more severe symptoms when they hemorrhage.
Also Check: Angels In Sign Language
Are Other Treatments For Cavernous Angioma Available
Doctors have treated cavernous angioma with stereotactic radiosurgery, also known as gamma knife, linear accelerator, X Knife, Brainlab, or cyberknife, for many years, but its effectiveness is not clear. In stereotactic radiosurgery, focused radiation is directed at the cavernous angioma without opening the skull. Experts now recommend that radiosurgery be considered only with individuals who have a single symptomatic lesion that is in an area of the brain where the risks of traditional surgery would be too high. Radiosurgery should not be used for treating cavernous angiomas that do not cause symptoms or for cavernous angioma in people with the hereditary form of the illness, as the radiation itself might trigger new cavernous angiomas to form. Other minimally invasive surgical techniques are being used more widely.
Researchers are working to find medications to treat cavernous angiomas. It may take more than one medication to treat every situation. Medications could be useful to:
Who Might Be Involved In My Care
- NEUROLOGIST manages symptoms like seizure and pain
- NEUROSURGEON evaluates for surgery
- REHABILITATION SPECIALISTS improve functioning after brain event
- ORTHOPEDIST monitors spine in CCM3 patients
- NEURO-OPHTHALMOLOGIST cares for brain-related vision problems
- GENETICIST evaluates for the hereditary form of the illness
- DERMATOLOGIST cares for vascular skin lesions in hereditary illness
Also Check: Guinea Pig Ear Cleaning
Dva With Cavernous Angioma
In 2004, Vern, then a 28-year-old father of two, hit his head while practicing jujitsu. From the subsequent CT scan, Vern and his wife Tiffany were surprised to learn that Vern had a more serious and long-term condition. Doctors diagnosed him with multiple cavernous angiomas surrounding a large developmental venous anomaly , a dilated malformed vein, in his brainstem. While a DVA by itself typically does not cause symptoms or complications, Verns DVA had set the stage for the development of more than one cavernous angioma.
It was not until two years later that Vern had his first hemorrhage. As a result, he closed his business as a mobile fleet service mechanic to focus on his recovery and his family. I couldnt drive, Vern explains. My reaction time was just not near what it needed to be to operate a vehicle safely. Vern is driving again, but not on interstates or during times of heavy traffic. He also has been recovering from gait and vision deficits.
Vern has consulted numerous surgeons about removing the most problematic of his cavernous angiomas. The DVA complicates surgery. Verns wife Tiffany explains, The angioma that keeps bleeding is located too close to his DVA to remove. The DVA looks almost like a hook, and the angioma is on the inside of that hook. Disturbing a large DVA like Verns can cause a catastrophic stroke.
What Are Developmental Venous Anomalies
A developmental venous anomaly is an unusual or irregular arrangement of small veins that may look like the spokes of a wheel. The veins drain into a larger central vein. DVAs are benign .
DVAs also may be called venous angiomas or benign variations in venous drainage. Some doctors refer to them as caput medusae, a Latin term that means head of Medusa because the clump of veins resembles snakes on the head of the Greek mythological character named Medusa.
These unusual vein formations can occur anywhere in the body but are found most often in the brain or spinal cord. By some estimates, as many as 1 in 50 people has at least one DVA.
Also Check: Teach Myself Sign Language
There Exist Several Clinically Detectable Causes Of Pt
The most striking finding to come out of this review is the expansive breadth and depth of pathologies that are causal-for, or at least common correlates-of PT. These conditions range from the benign to the life threatening, and stem from genetic defects, chronic diseases, and/or acute injuries. Tables 1-3 summarise the types and frequencies of PT-related conditions identified in our reading. Generally speaking, a glomus tumour or similar will be visible in the middle ear , while auscultation of the scalp, neck and eyes will often indicate that some form of arterio-venous fistula is present . PT in a young, obese, commonly female patient will lead to a suspicion of BIH . A hyperdynamic circulatory state can be suspected after a physical examination . There remains a group of patients for whom no diagnosis is suggested by either the history or the clinical examination and although, in theory, these may have a detectable underlying cause, many are truly idiopathic.
Table 4
The middle ear
Arterial abnormalities
Venous causes
Suggested causes of venous PT include a high riding jugular bulb, sigmoid sinus arachnoid granulation, abnormal condylar or mastoid emissary veins, and abnormal venous collaterals . These latter conditions have been found in conjunction with venous PT, but a cause and effect relationship has not been established. The natural history of these conditions is not one associated with morbidity.
BIH
Table S2
Rare associations
Causes Of Venous Angioma
The most likely and frequently occurring causes of venous angioma are:
- Genetic genesis of pathology.
- The consequences of an infectious disease of the patient.
- Trauma received in the head region.
As observations show, if there is no trauma, heredity comes first. Infection damage, leading to the development of an interesting pathology, is rare, but it should not be excluded from the accounts.
, , , ,
Read Also: Connecting Phonak To Iphone
How Are Developmental Venous Anomalies Diagnosed
Developmental venous anomalies have no symptoms and may only be found when you have imaging tests to look for the cause of other health problems. Imaging tests may include MRI or MRA, conventional angiogram, or specific types of CT scans that show areas of blood flow.
Most people may never know they have a DVA, and it will only be found after their death, if an autopsy is done.
Venous Frontal Lobe Angioma
Depending on the location of the tumor, the patient feels a slightly different set of symptoms. At the same time, a number of signs are common to all pathological manifestations, and a number gives off individuality. Venous frontal lobe angioma can be manifested:
- Dizziness and pain in the forehead.
- The appearance of a convulsive syndrome.
- Epileptic seizures are possible.
- Unconsciousness in actions.
- Problems in walking, vertical stability of the body.
The frontal lobes of the brain are responsible for the manifestation of interest, responsibility, the ability to make informed decisions, initiative. With changes in this area, there is a transformation of these opportunities, which is expressed by the pathological symptom described above.
You May Like: Teach Yourself Sign Language
Mri Is The Most Sensitive Imaging Modality For Diagnosing Pt
If imaging is indicated, ideally it will be cost-effective, comprehensive, non-invasive and radiation free. MRI is best suited for this and over the last decade has become far more accessible. Cost remains higher than CT, though its superior contrast resolution and sensitivity for a wider spectrum of pathology justifies this difference. MRI with contrast can often be the sole imaging investigation.
Imaging should be directed by clinical findings and medical history
A thorough understanding of the various etiologies associated with PT is invaluable for the clinician involved in the initial assessment of a PT patient. A through physical examination and comprehensive medical history will direct the clinician to a specific hypothesis, facilitating the choice of an appropriate approach to diagnostic imaging .
In taking the medical history, it is important to note risk factors including head trauma, tumours, and any cardiovascular issues, e.g., coronary artery disease or hypertension, comorbidities such as vertigo, hearing loss, aural fullness, headache or neck ache, and any observable fluctuations in the PT . Does the PT worsen after exercise or when lying down? The patient should be asked to describe the perceived intensity of the PT, and an inquiry should be made as to the specific reason for their visit. That is, has the intensity of the symptom acutely changed, does the symptom seem to be gradually worsening, or has a new symptom recently developed?
Radiological findings
Do I Need Genetic Testing
Most people with a cavernous angioma do not need genetic testing. We believe only 25% of individuals with a cavernous angioma have a hereditary form of the illness. If you have just one cavernous angioma, you need an MRI with special imaging called susceptibility-weighted imaging to rule out the hereditary form. If you have multiple cavernous angiomas but you also have a developmental venous anomaly , SWI will show whether your lesions cluster near the DVA or whether they are in other areas of your brain. If the cavernous angiomas are only around the DVA, you do not need testing. Having multiple cavernous angiomas clustered around a DVA is typical of the sporadic form of cavernous angioma. You cant inherit or pass down the sporadic form of the illness. People who have multiple cavernous angiomas that are not associated with a developmental venous anomaly should request genetic testing. Sometimes people are the first in their family with a hereditary form. You do not need other affected family members to justify testing.
Read Also: Guinea Pig Ear Wax